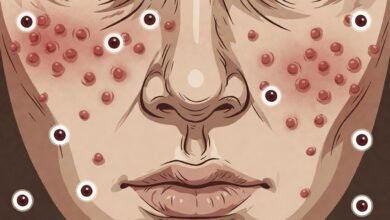
Fungal Acne: How to Spot It, Treat It, and Keep It From Coming Back
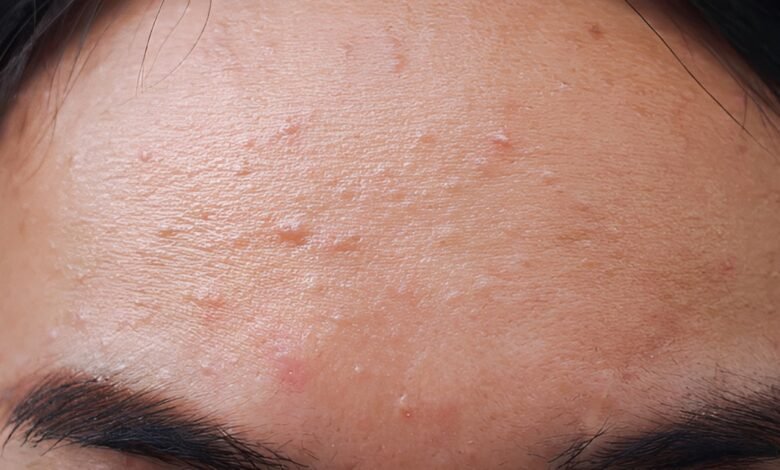
Small bumps on one’s skin that incessantly itch and do not respond to “regular” acne treatment may be fungal acne. Many people mistake this condition for “regular” acne and consult incorrect remedies, only to be more irritated than before. With the right understanding and therapeutic remedies, more people can cure this condition for good.
Fungal acne, in itself, isn’t real acne. Rather, it is classified as a type of folliculitis caused by a yeast overgrowth. Bacterial acne results from clogged pores and inflammation caused by Cutibacterium acnes. On the other hand, folliculitis is caused by Malassezia yeast. This yeast feeds on the skin’s natural oils and is found in warm, moist environments. It converts “harmless” hair follicles into red bumps.
What Fungal Acne Really Looks Like
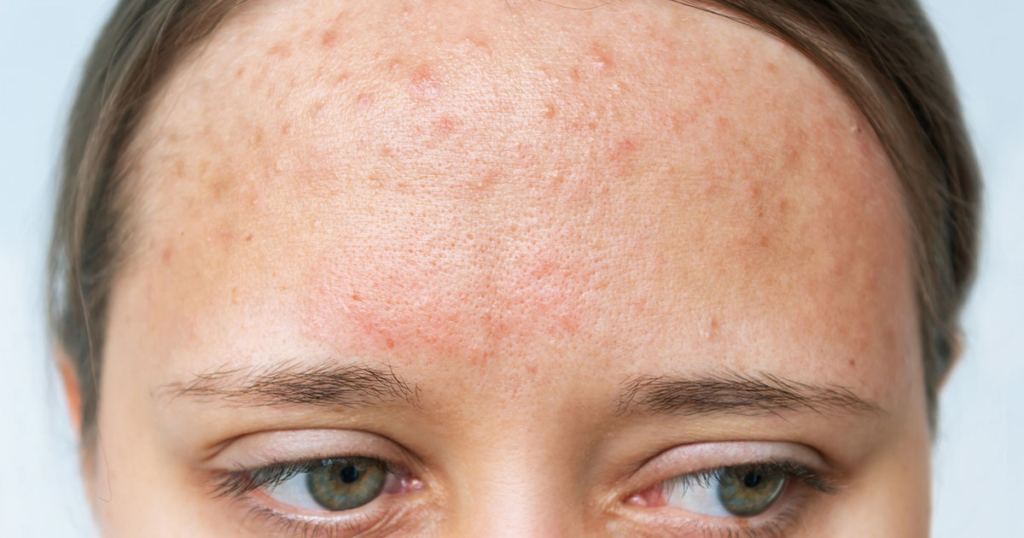
Fungal acne appears in clusters on the chest, back, shoulders, and even the forehead and hairline. They are the same size, and they appear as tiny, flesh-coloured or pink bumps that feel rough. Most people say they have more itch than pain, especially after sweating or in hot, humid conditions.
They lack the characteristics of blackheads and whiteheads. Where regular acne can present with several types of lesions, fungal acne features small, consistently monomorphic bumps with little or no pus. A breakout that looks like a rash of identical pimples is a classic case, especially after a sweaty workout or vacation in the tropics.
Skin texture changes, too. Areas affected by the yeast can become prickly and even develop a sandpaper feel, especially if the yeast has been active. Several moisturisers can also make things worse, as yeast is often found in them.
Why Does Fungal Acne Keep Coming Back?
There are many reasons sweaty, humid skin is susceptible to this fungus, leading to pimples popping up and the fungus spreading. First, the yeast responsible for this skin condition thrives in warm, moist environments. This is why athletes, individuals living in warm regions, and people who wear tight synthetic clothing as part of their workout routine are most impacted.
Some medications reduce the body’s ability to control this yeast, allowing it to overgrow, which can lead to pinched inflammation and infection. For example, antibiotics can eliminate the small amount of beneficial bacteria in the body that help control yeast. In addition, birth control and pregnancy can lead to increases in oil production due to hormonal improvisation, which creates a home for the yeast to grow. In addition, higher cortisol levels from stress can lead to increased sebum production, which often fuels this condition.
Your skin and hair products can also affect your skin condition. For example, many popular acne treatments contain coconut and olive oil, which are highly nourishing to the skin. Also, many products with thick, creamy textures can create a perfect environment for yeast to grow. Therefore, many people who switch to more “natural” andsafe products to improve their skin condition often make their condition worse because of this concern.
Even though the correlation isn’t as strong as with bacterial acne, diet can still play a role in fungal acne. Sugary and carb-heavy foods can spike insulin levels, which can lead to increased oil production and food for the yeast on the skin. The most concerning diet triggers in this case are fermented foods and other foods that generally promote higher yeast production in the body.
What makes fungal acne different from regular acne
Most people are confused by this. Typical acne medications, such as retinoids, salicylic acid, and benzoyl peroxide, can make fungal acne worse by drying out the skin and disrupting the microbiome. If you notice that your spots are getting redder and itchier while using these, that is a strong sign that you are treating the wrong thing.
Location is also a hint. Bacterial acne tends to have a strong predilection for the forehead, jawline, and chin. These areas are oilier and are influenced by hormones. In contrast, fungal acne is commonly found on the upper body and chest, back, and sometimes the outer arms.
Itching is another clue. Regular pimples might sting or feel tender, but they rarely itch intensely. Fungal acne almost always comes with that annoying, persistent itch that makes you want to scratch, even when you know you shouldn’t.
The Story of Healing Patterns
Different types of body acne have distinct healing patterns. For example, acne on the body caused by bacteria rarely heals without leaving behind a mark or a scar. However, fungal acne doesn’t usually leave scars, and once you treat it with the appropriate antifungals, it tends to heal uniformly and doesn’t leave behind post-inflammatory pigmentation.
Getting the Correct Diagnosis
Most dermatologists can identify fungal acne with a quick visual exam. In some cases, though, they may perform a quick test in which a small scraping is taken for microscopic examination to determine whether yeast is present. When there is no improvement, a biopsy can rule out other conditions, such as eczema or bacterial folliculitis.
You can often begin making progress without a doctor’s visit. If your body acne matches the description: itchy, uniform bumps on the torso and does not respond to acne treatments, there is a high probability that it is fungal acne. If you suspect your acne may be resistant to treatment, you should seek professional help.
Treatments that Work
The first step of treating fungal acne is to begin using topical antifungal agents. Do not use any antibacterial products, as this will make your skin more sensitive and only aggravate the condition. Ketoconazole shampoo really works. Yes, the shampoo that is used for dandruff. You can also use it as a body wash two to three times a week and let it sit on the affected areas for five minutes. The active ingredient targets Malassezia yeast and usually shows results within a week.
Sulfur washes also really work. Try to get washes with a sulfur content of 5-10%. These kinds of washes dry out the yeast without damaging your skin barrier, unlike more intense treatments. Many people use sulfur washes combined with a gentle salicylic acid cleanser to keep pores clear while eliminating fungus.
On the other hand, prescription creams like Clotrimazole and Econazole work to target the issue more quickly. For breakouts that are more widespread and recurring, we can use oral antifungals like Fluconazole or Itraconazole. These medications come as a short prescription and can clear the stubborn fungal acne really fast.
It is also important to maintain the skin’s defences. Probiotic supplements, especially those containing Saccharomyces boulardii, can help balance yeast levels. Some dermatologists recommend these supplements, along with topicals, to achieve better results.
Natural Strategies That Make a Real Difference
When it comes to fungal acne, the main focus is definitely medical treatments; however, modifying your wardrobe and shower habits can help reduce the likelihood of recurrence and make it less problematic when it does. For your clothing, try to pick out and wear items made of natural fibres (like cotton and bamboo) because they allow your body to breathe and help wick moisture, which reduces the level of yeast-generated moisture. If you need to do a longer workout, make sure to wear your tighter polyester athletic clothing and change afterwards to minimise the time you spend in
Shower as quickly as you can afterwards to keep the yeast and moisture from multiplying. Do a quick body wash with an antifungal wash to reduce the yeast within seconds. Be sure to do these rinses really well, especially in areas of your body, like the back and chest, that are easy to forget, as these are usually places where you can develop yeast and acne.
When it comes to hair, you should also consider the effects of your hair care. If you choose to use a heavy conditioner, it will run down the back and add to the feeding of the problem, and that has to be your back, hair, and body wash. Do consider using a lot of light and rinsable conditioners, because that helps a lot.
Additionally, when treating fungal acne, make sure to cover the areas of skin that will be exposed to the sun with a light, mineral, non-comedogenic, oil-free sunscreen. Many sunscreens and antifungals can cause your skin to burn.
The Skin Care Routine You Need to Avoid Fungal Acne
The most important element of a skincare routine to avoid fungal acne is to keep it simple. Focus on balancing the skin’s natural barrier rather than stripping oils, which can cause the skin to produce more oil.
Cleansers are one of the most important steps in a balanced routine, and using a sulfate-free, pH-balanced face wash is the best option. Your face wash should not irritate the skin, cause it to produce more oil, or wash away the moisture locks the skin provides.
Try to avoid physical exfoliants and instead choose gentler chemical exfoliants, such as lactic acid, mandelic acid, or others. You don’t want to irritate the skin and disrupt the microbiome too much.
Active ingredients should be limited to proven antifungal agents, such as diluted tea tree oil or zinc pyrithione, the latter of which is found in many antifungal dandruff shampoos.
Improvement is expected in the first 10 days, and after that, the skin should continue to clear and finally be free of fungal acne after 4-6 weeks, once the activity is over. The first improvement usually occurs when the itching subsides, and the bumps on the skin flatten.
In the clearing phase, you’re most likely to experience purging, when your skin looks worse than before. This is simply because there is likely a yeast infection on the skin, and dead skin and other debris need to be cleared. Stick to the routine and bear with this phase, because it is likely to lead to the clearest skin most of us have had in a long time.
If, with time and patience, bumps clear and new bumps keep appearing despite changing the routine, it is time to consider the environment and other outside factors that may still be activating the yeast infection. This may include the laundry detergent, the humidifier, or your pillow. There is probable cause, and eliminating these external factors, including your environment, will help you pinpoint the most likely cause.
Once you have cleared the infection, the goal is to keep the yeast at bay. Staying consistent with breaking the routine will be beneficial. Breaking routine and washing with antifungal soap will be beneficial, especially for a non-existent yeast infection.
It is now time to keep a close watch on the changing seasons. It is now time to keep a close watch on the changing seasons. It is time to keep a close watch on the changing of the seasons. It may be necessary to shower more and then use a product to help you dry off as completely as possible. Summer humidity will bring back more problems.
Did you know that your skin and gut health are connected? Improving your gut health by eating more fermented, fibre-rich, and anti-inflammatory foods can also benefit your skin. Fermented foods help your microbiome. A balanced microbiome helps maintain your yeast immune system. Some people report that cutting dairy and refined sugars helps their skin. However, this can vary a lot from person to person.
Managing your stress helps keep your body and skin healthy. Chronic stress keeps your body running high in cortisol all the time. This can make your skin produce more oil and cause fungal infections. You may not think about it, but small, simple changes can make a big difference! Changes such as taking short walks each day, using meditation apps, or even making sure to get enough sleep can help you avoidavoid skin infections.
In Summary
You may feel like you are struggling and fighting with your skin. However, fungal acne and other skin infections can be easy to deal with once you know what to do. It is important to treat the underlying cause of the infection rather than just treating the yeast on your skin.
You can get your skin to be clear and calm by making a few changes to your antifungal treatments, what you use on your skin, and g a few little changes in your life. You may have to try a few things, but seeing the small improvements in your skin is very worth it.
Patience is most crucial. Just as it took time for the overgrowth to develop, it will take time and effort to keep it under control. However, you can find hope in the fact that many have successfully reclaimed their skin from fungal acne. So, you can do it too.
You may also read itbigbash.